Doctors and researchers have observed an improvement in the survival rate of cancer patients when they are given a combination of a chemotherapeutic drug (cancer-killing drug) and an antiangiogenic drug (a drug that inhibits the growth of new blood vessels). This combination treatment seems to give patients a better chance of surviving than just chemo alone. It has not been clear why antiangiogenic drugs help patients undergoing chemotherapy, but cancer researchers have recently published a study in PNASProceedings of the National Academy of Sciences that sheds some light on the matter.
Chemotherapeutic Drugs
Cancer chemotherapy involves the administration of toxic chemicals that are intended to target and kill cancer cells. Unfortunately, no chemotherapeutic agent has perfect selectivity for malignant cells, so the rest of the body is slowly poisoned even as the chemicals work to kill tumors. For this reason, chemotherapy is usually very difficult for a cancer patient. A substantial number of patients can actually die because of chemo’s negative side effects.
Here are a couple of examples of chemotherapeutic drugs – these are the ones used in this study.
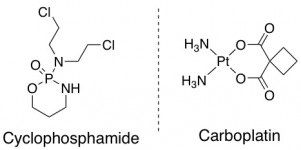
Antiangiogenic Drugs
The second type of drug discussed in this study is an antiangiogenic drug. Unlike chemo drugs, antiangiogenics aren’t particularly toxic to cells (cancerous or non). Instead, they act to prevent the growth of new blood vessels (arteries, capillaries, and veins).
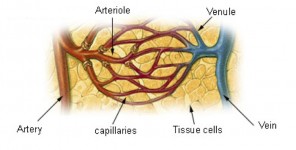 Blood vessel growth has an interesting role in cancer. Tumor cells are notorious for being able to get new capillaries to grow toward them; these provide nutrient-rich blood to help the cancer cells thrive. Thus you can imagine that an antiangiogenic drug would make it harder for a tumor to grow, since it would have a difficult time getting new blood supplies to come its way. But slowing tumor growth is not the same as actually killing tumor cells.
Blood vessel growth has an interesting role in cancer. Tumor cells are notorious for being able to get new capillaries to grow toward them; these provide nutrient-rich blood to help the cancer cells thrive. Thus you can imagine that an antiangiogenic drug would make it harder for a tumor to grow, since it would have a difficult time getting new blood supplies to come its way. But slowing tumor growth is not the same as actually killing tumor cells.
Here is an example of an antiangiogenic drug – this is sunitinib, the drug used in this study.
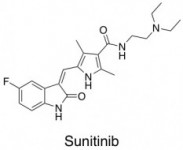
Effect of Each Drug On Its Own
Chemo drug: carboplatin. Some mice with cancerous tumors were treated with carboplatin (and nothing else), and – sadly – about 80% of them died within 10 days, apparently from the side effects of this drug. Over the 10 days, their tumors had been shrinking though.
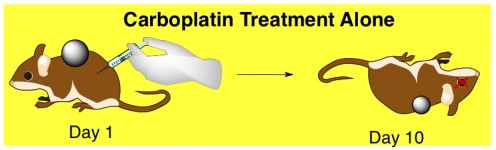
Antiangiogenic drug: sunitinib. Some more mice with cancerous tumors were treated with sunitinib (and nothing else). After 10 days, they were all still alive, though their tumors hadn’t shrunk at all.
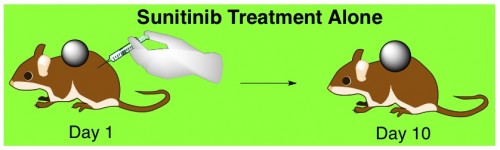
Effect of the Two Drugs in Combination
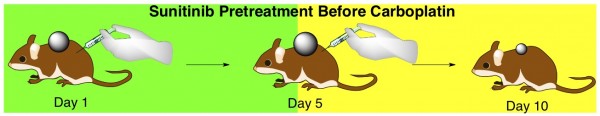
The researchers gave tumor-bearing mice sunitinib for 5 days. Then they took the mice off of this antiangiogenic drug and gave them carboplatin for the next 5 days.
The mice that had this 5-day treatment with sunitinib prior to initiation of chemotherapy with carboplatin had a better survival rate than those not pretreated with sunitinib. Furthermore, the combined sunitinib + carboplatin treatment led to greater tumor shrinkage than just carboplatin with no pretreatment.
Mechanism of Action
Tumor cells are able to attract a blood supply in their direction by causing an increase in the levels of a protein called VEGFvascular endothelial growth factor. The presence of this protein signals the body to grow new blood vessels. Cancer patients often have measurably high levels of VEGF circulating in their bodies, and these elevated levels can impair the function of several tissues and organs. One of the things too much VEGF does is prevent the production of blood cells in bone marrow.
The scientists performing this mouse study found that chemotherapy (with carboplatin) exacerbates the effects of the already-high levels of VEGF, often resulting in a fatal loss of bone marrow function.
Antiangiogenic drugs like sunitinib are able to block VEGF. Therefore, pretreatment of the mice with VEGF-blocking sunitinib served to protect bone marrow from the upcoming chemotherapy.
Take-Away Message
This study suggests that pretreatment with antiangiogenic drugs before chemo drugs is more effective than the traditional concurrent treatment with both drugs.
Citation:
Zhang, D., Hedlund, E., Lim, S., Chen, F., Zhang, Y., Sun, B., & Cao, Y. (2011). Antiangiogenic agents significantly improve survival in tumor-bearing mice by increasing tolerance to chemotherapy-induced toxicity Proceedings of the National Academy of Sciences DOI: 10.1073/pnas.1016220108


5 Responses to Blood Vessel Growth Inhibitors Mediate Negative Side Effects of Chemotherapy